Understand that combining CBD with central nervous system (CNS) depressants or alcohol creates a serious risk of amplified sedative effects that can impair your coordination, judgment, and breathing. CNS depressants—including benzodiazepines like Ativan, sleep medications like Ambien, opioids, and certain muscle relaxants—slow down brain activity, and CBD may intensify these effects through shared metabolic pathways in your liver. When you add alcohol to this equation, you’re layering another depressant that compounds the danger.
Check your current medications against known CBD and medication interactions before starting any CBD regimen, particularly if you take prescription CNS depressants. The CYP450 enzyme system in your liver processes both CBD and most CNS depressants, meaning CBD can slow down how quickly your body eliminates these medications, potentially leading to dangerously high blood levels.
Space out your CBD and alcohol consumption by at least several hours, and never combine CBD with alcohol if you’re already taking prescription CNS depressants—this triple combination significantly increases your risk of severe sedation, respiratory depression, and accidents. I’ve spoken with countless Canadians who assumed CBD’s natural origins made it risk-free, only to experience unexpected drowsiness or dizziness when mixing it with their evening glass of wine or anxiety medication.
Consult your healthcare provider or pharmacist before combining CBD with any CNS depressant medication, as they can assess your specific situation and adjust dosages accordingly to minimize interaction risks.
What Are CNS Depressants and Why Should You Care?
Common Types of CNS Depressants
Understanding which medications fall into the CNS depressant category is crucial when considering CBD use or alcohol consumption. Let me break down the main types you’re likely to encounter in Canada.
Benzodiazepines are among the most commonly prescribed CNS depressants. These medications treat anxiety, panic disorders, and insomnia. You might recognize brand names like Ativan (lorazepam), Xanax (alprazolam), or Valium (diazepam). Many Canadians also take Rivotril (clonazepam) for seizure control or anxiety management.
Barbiturates, while less common today, are still prescribed in certain situations. These older medications include phenobarbital, sometimes used for seizure disorders. They’re much stronger than benzodiazepines and carry higher risks.
Sleep medications represent another significant category. Beyond benzodiazepines used for sleep, there are newer options like Imovane (zopiclone) and Sublinox (zolpidem), which many Canadians take for insomnia. These work similarly to benzodiazepines in slowing brain activity.
Muscle relaxants help manage pain and muscle spasms. Common examples include Flexeril (cyclobenzaprine), Robaxin (methocarbamol), and Zanaflex (tizanidine). I’ve spoken with several people who didn’t realize their muscle relaxant could interact with other substances because it seemed relatively mild.
Certain pain medications also depress the central nervous system, particularly opioids like morphine, OxyContin (oxycodone), and Tylenol 3 (codeine with acetaminophen). Even some over-the-counter medications like Gravol (dimenhydrinate) have CNS depressant properties.
If you’re taking any of these medications, it’s essential to discuss potential interactions with your healthcare provider before adding CBD to your routine or consuming alcohol. Your pharmacist can also provide valuable guidance specific to your prescriptions.
How CNS Depressants Affect Your Body
To understand how CNS depressants interact with substances like CBD or alcohol, let’s first talk about what they actually do inside your body.
CNS depressants work by slowing down your central nervous system, which includes your brain and spinal cord. Think of your brain as having an accelerator and a brake pedal. CNS depressants essentially press down on that brake, reducing the rapid-fire communication between nerve cells.
The main way they do this is by enhancing a neurotransmitter called GABA (gamma-aminobutyric acid). GABA is your brain’s natural calming chemical. When CNS depressants boost GABA activity, they create a cascade of effects throughout your body: your racing thoughts slow down, physical tension melts away, and that anxious feeling in your chest eases up.
This is why doctors prescribe these medications for anxiety disorders, sleep problems, and muscle spasms. The sedative effects can be genuinely helpful when you need them. Your breathing becomes slower and deeper, your heart rate decreases, and your muscles relax. For someone struggling with panic attacks or severe insomnia, these effects can be life-changing.
However, here’s what’s important to understand if you’re considering mixing CNS depressants with other substances: this slowing effect doesn’t just target the parts of your brain you want to calm down. It affects your entire nervous system, including the parts that control essential functions like breathing and heart rate. This is exactly why understanding potential interactions becomes so crucial for your safety.
How CBD Works in Your System
The Liver Connection: Why CBD Affects Other Medications
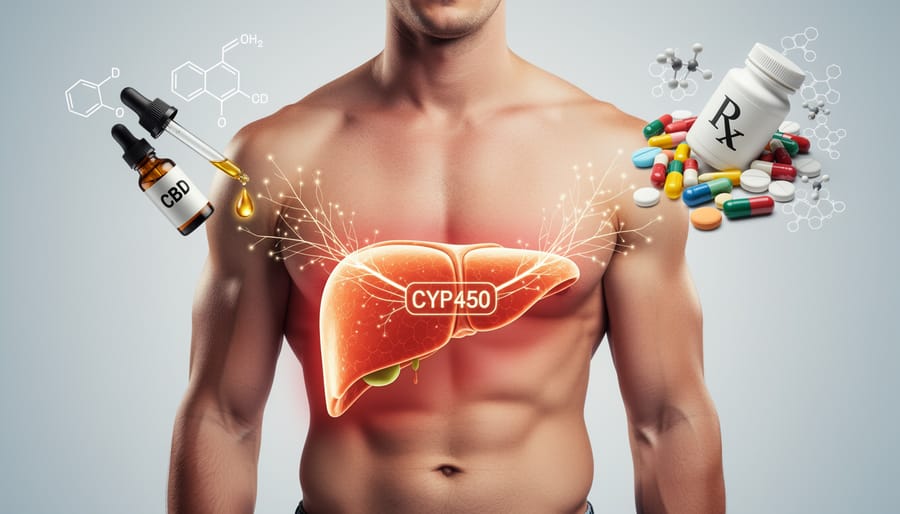
When I first learned about how CBD affects medications, I was honestly surprised by the science behind it. The connection happens in your liver, where a family of enzymes called cytochrome P450 (often shortened to CYP450) does the heavy lifting when it comes to breaking down substances in your body.
Think of these enzymes as tiny workers in a factory, processing everything from medications to alcohol. Your liver contains dozens of different CYP450 enzymes, but CBD specifically inhibits several key ones, particularly CYP3A4 and CYP2C19. These two enzymes alone are responsible for metabolizing roughly 60% of all prescription medications available in Canada.
Here’s where it gets important for your safety: when CBD temporarily slows down these enzymes, any medications that rely on them for breakdown will stay in your bloodstream longer than expected. Instead of being processed at the normal rate, the drug concentration builds up, potentially amplifying both therapeutic effects and side effects.
For CNS depressants specifically, this can be particularly concerning. If your body can’t metabolize your anxiety medication or sleep aid at the usual pace, you might experience stronger sedation, increased drowsiness, or impaired coordination without realizing why. The same dose you’ve taken safely for months could suddenly feel much more powerful.
The grapefruit effect is a helpful comparison many people recognize. Grapefruit juice inhibits similar liver enzymes, which is why doctors warn against mixing it with certain medications. CBD works through a comparable mechanism, just with different enzymes involved. Understanding this liver connection helps explain why timing, dosage, and medical supervision matter so much when combining CBD with other substances.
The Real Risks: CBD and CNS Depressant Interactions
What Happens When You Combine Them
When you mix CNS depressants with alcohol, you’re essentially doubling down on sedation. Both substances work on similar pathways in your brain, slowing down your central nervous system. The problem? This isn’t a simple case of one plus one equals two. The combined effects often multiply rather than just add together, creating what doctors call a synergistic or additive effect.
In practical terms, here’s what this looks like: imagine you’ve taken a prescription benzodiazepine for anxiety and then have a couple of glasses of wine. You might expect to feel a bit more relaxed than usual, but what actually happens can be much more dramatic. People often experience extreme drowsiness that comes on suddenly, difficulty staying awake even when trying, and significant impairment in coordination and judgment.
The real-world effects can be quite concerning. Your breathing may slow to dangerous levels, especially during sleep. You might feel confused or disoriented, struggle to form clear memories of what happened, or experience severe dizziness that makes even simple tasks risky. Some people describe feeling detached from reality or having slurred speech that’s far worse than either substance would cause alone.
I’ve heard from readers who thought they were being careful by spacing out their medication and drinks, only to wake up the next morning with no memory of the evening. Others have described frightening moments of not being able to catch their breath properly or losing their balance and falling.
The danger escalates quickly because these combined effects can impair your ability to recognize you’re in trouble.
Signs You’re Experiencing a Dangerous Interaction
Knowing the warning signs of a dangerous interaction can literally save a life. When CNS depressants and alcohol combine in your system, your body will often send clear distress signals that shouldn’t be ignored.
Watch for these critical warning signs:
Extreme drowsiness or difficulty staying awake is one of the first red flags. If you or someone else can’t keep their eyes open or seems unusually sedated beyond normal tiredness, this indicates excessive central nervous system suppression.
Difficulty breathing or slowed breathing is perhaps the most dangerous sign. If breathing becomes shallow, slow, or irregular, this is a medical emergency. The respiratory system is shutting down, which can quickly become life-threatening.
Confusion or disorientation beyond typical intoxication is another serious concern. This might look like not recognizing familiar people or places, extreme difficulty forming coherent sentences, or being unable to respond to simple questions.
Loss of coordination that goes beyond stumbling can signal serious trouble. We’re talking about complete inability to walk, stand, or control body movements.
Other concerning symptoms include bluish lips or fingertips (indicating oxygen deprivation), vomiting while unconscious or semi-conscious, seizures, or complete unresponsiveness.
When to seek help: If you notice any combination of these symptoms, call emergency services immediately. In Canada, dial 911 without hesitation. Don’t try to “sleep it off” or wait to see if symptoms improve. The Good Samaritan Drug Overdose Act protects you from simple possession charges when calling for help during an overdose, so never let legal concerns delay getting medical attention. Time is absolutely critical in these situations.

CBD and Alcohol: A Risky Combination?
What the Research Actually Says
Here’s what we actually know from research – and I’ll be honest with you, there’s less solid data than we’d like. Most studies examining CBD and alcohol interactions have been conducted on animals or in small human trials, which means we need to be cautious about drawing firm conclusions.
Some early research suggests that CBD might actually reduce blood alcohol levels when taken together, though the clinical significance of this isn’t entirely clear. A few small studies have also explored whether CBD could protect against some of alcohol’s negative effects on the brain and liver, but these findings are preliminary at best.
What we know more confidently is how each substance works independently. CBD interacts with your endocannabinoid system and can affect certain liver enzymes that metabolize medications. Alcohol is a well-established CNS depressant with predictable effects on the brain and nervous system. The challenge is that we don’t have extensive human trials examining what happens when you combine them regularly.
As for CBD with prescription CNS depressants like benzodiazepines or sleep medications, the research is even more limited. We know both can cause drowsiness and that CBD affects drug metabolism, but large-scale studies specifically tracking these interactions in humans are lacking.
This doesn’t mean combining these substances is automatically safe or dangerous – it means we’re working with incomplete information. That’s exactly why talking to your healthcare provider becomes so important, especially if you’re taking prescription medications.
The Enhanced Sedation Effect
When you combine CBD with alcohol, you’re essentially stacking two substances that both slow down your central nervous system. Think of it like pressing the brake pedal twice – the effect becomes much stronger than either substance alone.
I’ll be honest with you – I’ve heard from several people in the Canadian CBD community who didn’t realize how intensely CBD could amplify their usual glass of wine. One person told me they felt unusually drowsy after having their regular evening drink with their new CBD routine, something they hadn’t anticipated at all.
Here’s what happens: CBD can enhance alcohol’s sedating properties, potentially leading to significantly greater impairment than you’d expect. You might experience increased drowsiness, more pronounced loss of coordination, and diminished motor control. That beer or cocktail that normally just helps you relax could leave you feeling much more intoxicated when CBD is in the mix.
The concern isn’t just about feeling sleepier than usual. This enhanced sedation can affect your judgment, reaction time, and physical coordination in ways that could be dangerous. Activities that require alertness – like driving, which is subject to strict impaired driving laws across Canada – become considerably riskier.
The tricky part is that this interaction can vary significantly from person to person. Factors like your body weight, tolerance to either substance, the CBD dosage you’re taking, and how much alcohol you consume all play a role. What feels manageable for one person might be overwhelming for another, making it difficult to predict your personal response.
Danielle’s Take: My Experience and What I’ve Learned
I’ll be honest with you – this topic hits close to home because I’ve had countless conversations with Canadians who’ve reached out asking about mixing CBD with their evening glass of wine or their prescribed anxiety medications. Over my years researching and using CBD, I’ve learned that the answers aren’t always black and white, but they’re incredibly important.
One conversation that sticks with me was with my own doctor when I first started using CBD while occasionally enjoying a drink. She explained that even though CBD is generally well-tolerated, combining it with alcohol or medications that slow down your central nervous system creates a compounding effect. Think of it like stacking blankets – one might be comfortable, but too many can feel suffocating.
What I’ve learned through both personal experience and feedback from readers across Canada is that timing matters enormously. Several people have shared that they space out their CBD use and any CNS depressants by at least a few hours, always after consulting their healthcare provider. One reader from Ontario told me she stopped her nightly CBD routine entirely after noticing increased drowsiness when combined with her prescription sleep medication.
The most valuable lesson? Never assume that natural means risk-free. I’ve made it a practice to keep detailed notes about how I feel when using CBD, especially if I’ve had alcohol or taken any medication. This information has been invaluable during doctor appointments.
My biggest piece of advice is simple: be your own advocate. Ask questions, keep your healthcare team informed about everything you’re taking, and pay attention to how your body responds. The Canadian healthcare providers I’ve spoken with appreciate when patients come prepared with specific questions about interactions rather than making assumptions.
Safe Practices: How to Use CBD Responsibly

Talk to Your Healthcare Provider First
Before combining CBD with CNS depressants or alcohol, it’s crucial to discuss with your healthcare provider. I learned this the hard way when I started using CBD for sleep while taking prescription medication. My doctor helped me understand the potential interactions and adjust my approach safely.
When booking your appointment, be specific about wanting to discuss CBD use alongside your current medications or alcohol consumption. In Canada’s healthcare system, you have the right to ask questions and receive clear answers. Bring a list of all substances you use, including dosages and frequency. Don’t leave anything out, even if you think it seems minor.
Ask your doctor about timing between doses, potential side effects to watch for, and whether any adjustments to your prescriptions might be necessary. Inquire about liver enzyme interactions, as both CNS depressants and CBD are metabolized similarly. Request guidance on safe CBD dosages and whether certain delivery methods are safer than others.
If your doctor seems unfamiliar with CBD, don’t hesitate to ask for a referral to someone more knowledgeable or request they consult with a pharmacist. Canadian pharmacists are incredibly helpful resources and can often provide detailed interaction information. Remember, advocating for your health isn’t pushy; it’s responsible. Your healthcare team should support your decision to explore CBD while ensuring your safety remains the top priority.
Timing and Dosage Considerations
If you’re taking CNS depressants and considering CBD, timing is everything. I learned this the hard way when I first started exploring CBD myself – jumping in without a clear plan left me uncertain about what was working and what wasn’t.
Start low and go slow is the golden rule here. Begin with the smallest possible CBD dose, typically 2.5 to 5 mg, especially if you’re on medications like benzodiazepines or sleep aids. This conservative approach lets you observe how your body responds without overwhelming your system. Wait at least 4 to 6 hours between taking your prescribed CNS depressant and using CBD when possible, giving each substance time to work independently.
Keep a simple tracking journal – it doesn’t need to be fancy. Note the time you take your medication, when you use CBD, the dose of each, and how you feel throughout the day. I use my phone’s notes app to record energy levels, drowsiness, mood changes, or anything unusual. This record becomes invaluable when discussing your routine with your healthcare provider.
Pay attention to cumulative effects. What feels fine on day one might feel different by day three as CBD builds up in your system. Give any new dosage at least a week before making adjustments.
Avoid using CBD and alcohol together, even in small amounts. The combined depressant effects can be unpredictable and potentially dangerous. If you do drink occasionally, skip your CBD that day.
Under Canadian law, you have access to legal cannabis products, but that doesn’t replace professional medical guidance. Your pharmacist can review your complete medication list and help identify potential timing conflicts specific to your prescriptions.
When to Avoid CBD Entirely
There are certain circumstances where combining CBD with CNS depressants or alcohol poses too great a risk and should be avoided altogether. If you’re taking high doses of benzodiazepines, opioids, or barbiturates for serious medical conditions, introducing CBD without medical supervision can be dangerous. The same applies if you’re in early stages of adjusting to a new CNS depressant medication—your body needs time to stabilize before adding another variable.
I’ve learned through conversations with healthcare providers that individuals with liver or kidney impairment should be especially cautious, as these organs process both CBD and most CNS depressants. Compromised function means substances stay in your system longer, increasing interaction risks.
Operating heavy machinery or driving is another absolute no-go zone when combining these substances. Even if you feel fine, your reaction times and judgment may be significantly impaired in ways you don’t notice.
If you’re struggling with substance use disorders or have a history of respiratory issues, avoid this combination entirely. The interaction between medications and CBD can be unpredictable, and in these vulnerable situations, the stakes are simply too high. When in doubt, always consult your healthcare provider before proceeding.
Canadian-Specific Considerations
In Canada, the regulatory landscape around CBD products is quite different from many other countries, which is something I’ve had to navigate personally over the years. Health Canada regulates CBD under the Cannabis Act, meaning all CBD products must be purchased from licensed retailers – either provincially-run stores, licensed private retailers, or authorized online sellers. This is actually good news for safety-conscious consumers because it means products undergo testing for contaminants, potency, and quality.
If you’re taking CNS depressants or consuming alcohol and want to use CBD, buying from licensed sources ensures you’re getting accurately labeled products. This matters because knowing the exact CBD content helps your healthcare provider give you better advice about potential interactions. I’ve learned to always check for the official Cannabis tracking label on products, which verifies they’ve come through the legal system.
For checking drug interactions, Canadians have several reliable resources. Your pharmacist is honestly one of the best starting points – they can access comprehensive drug interaction databases and are usually happy to discuss CBD. Many provinces also offer free telehealth services where you can speak with a nurse or doctor about concerns. Health Canada’s website provides general cannabis information, though it’s not always CBD-specific.
I’d also recommend the Canadian Pharmacists Association website, which has consumer resources about cannabis and medication interactions. If you’re already seeing a doctor for conditions requiring CNS depressants, they should be your primary consultation point before adding CBD to your routine.
Remember that even though CBD is legal in Canada, combining it with other substances that affect your central nervous system requires the same caution you’d use with any medication combination. The quality standards we have here give us a good foundation for safer use, but professional medical advice remains essential.
Looking back at what we’ve covered, I hope you now have a clearer picture of how CBD can interact with CNS depressants and alcohol. These interactions aren’t something to take lightly. When CBD affects how your body processes medications or amplifies the sedative effects of alcohol, the consequences can range from uncomfortable to genuinely dangerous.
The most important takeaway? Talk to your healthcare provider before combining CBD with any CNS depressants or alcohol, especially if you’re taking prescription medications. I can’t stress this enough. Your doctor or pharmacist knows your medical history and can give you personalized guidance that no article can replace.
From my own journey with CBD here in Canada, I’ve learned that being informed is empowering. Understanding how substances interact in your body isn’t about living in fear—it’s about making choices that respect your health and wellbeing. Yes, CBD offers incredible potential benefits for many Canadians dealing with anxiety, pain, and sleep issues. But those benefits are best experienced when you approach CBD use responsibly and with full awareness.
If you’re currently using CBD alongside other substances, don’t panic, but do take action. Schedule that conversation with your healthcare provider, be honest about what you’re taking, and adjust your approach if needed. Knowledge is your best tool for staying safe while exploring what CBD can offer you.


